Curious About Diastasis Recti? Dr. Samaha Answers Your Top 9 FAQs
Posted on July 26, 2024 | by Boston Plastic Surgery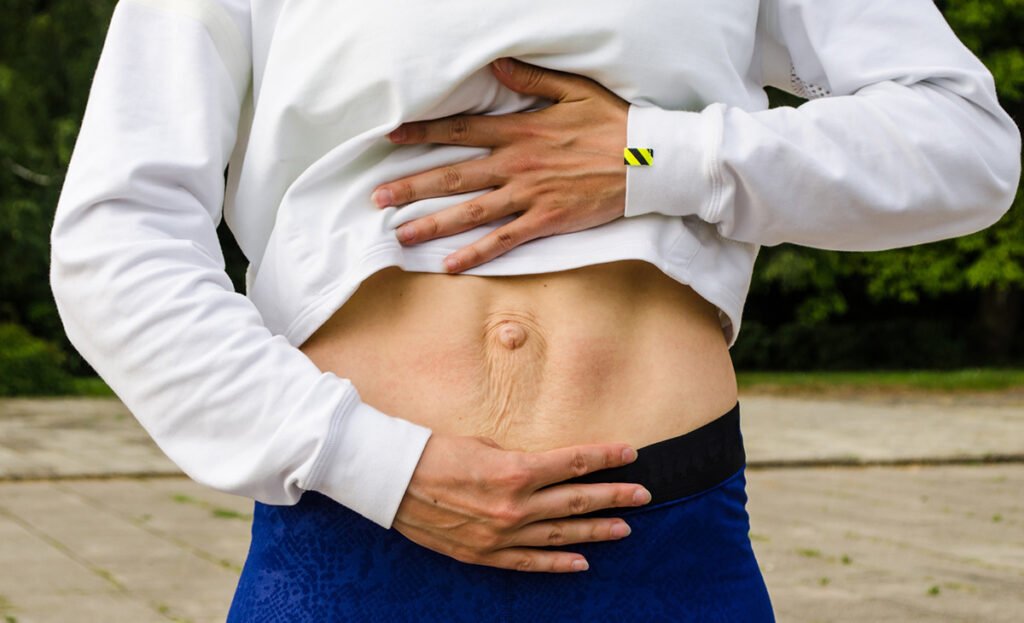
Pregnancy, childbirth, and even certain exercises can cause our abdominal muscles to weaken and separate, resulting in a protruding belly or “pooch.” This issue is called diastasis recti and is one of the most popular issues corrected during tummy tuck surgery. But despite its prominence, diastasis recti is largely misunderstood. In this post, board certified plastic surgeon and renowned diastasis recti reapir expert Dr. Fouad Samaha answers the top 9 questions you have about diastasis recti and shares his unique approach.
1. How common is diastasis recti?
Diastasis recti affects pregnant and postpartum women, overweight and obese people, and those with poor exercise technique. The condition is so common that an estimated 1 in 2 women experiences diastasis recti in their lifetime. Unfortunately, diastasis recti is often mistaken for a beer belly or excess weight gain; however, it’s a serious concern worthy of medical attention. Aside from looking unattractive, diastasis recti can contribute to lower back pain, constipation, bloating, pelvic floor imbalance, and poor posture, symptoms that often worsen if left untreated. Tummy tuck surgery, a.k.a. abdominoplasty, is typically performed to correct diastasis recti in a variety of patients.
2. Is surgery always needed to repair diastasis recti?
For severe diastasis recti that causes abdominal protuberance with or without associated functional problems, surgery is far superior to non-invasive techniques to definitively address the problem. I have had scores of patients that underwent physical therapy and other programs—sometimes for years—struggle with inadequate results and tell me, “I wish I had met you sooner. I should have done this years ago.”
Diastasis recti can cause lower back pain, poor posture, and even constipation & bloating, and can worsen if left untreated.
3. What types of sutures do you use in diastasis recti surgery?
The type of suture, or stitch, used to repair diastasis recti depends on the severity of a patient’s condition, their likelihood of re-developing the condition in the future, and a surgeon’s personal preference.
I typically use heavy, non-absorbable sutures to hold the abdominal muscles and fascia (the tissue that connects your abs) together and allow scar tissue to develop following diastasis recti surgery. These non-absorbable sutures are permanent in order to help prevent diastasis recti from reoccurring. Occasionally, I will use long-duration absorbable sutures in the second suture layer. (Read more about absorbable sutures and suture layers in Questions 5 & 6).
4. How do you determine where to place sutures?
When repairing diastasis recti, I place sutures deep beneath the skin and buried within the fascia, therefore they are never felt by the patient. For most diastasis recti repair, placing sutures vertically along the midline of the abdominal wall is adequate; however, if there is extensive fascia laxity, I may also place corset sutures along the obliques to provide support horizontally, and/or plicating sutures on either side of the belly button.
5. How many layers of sutures are required?
I like to use a 2-layered suture system to reinforce a patient’s fascia-to-muscle connection. The second layer of sutures not only provides extra support but also acts as a backup in the rare case the first layer was to tear. I prefer to use a series of “figure-of-eight” interrupted sutures for the first layer and a “running” suture for the second layer. I may sometimes place an additional third layer of sutures for extra support if a patient has an especially weak area of fascia.
6. Do the sutures dissolve? Can the patient feel the sutures?
Non-absorbable sutures are permanent, meaning they don’t dissolve, while absorbable sutures are designed to dissolve over time (usually after 4 months). Both types of sutures are proven to be safe and undetectable by the patient.
7. How do you address umbilical hernias when correcting diastasis recti?
In patients with diastasis recti, the abs are pulled apart and the fascia connecting them is weakened. Abdominal contents can poke through the thin fascia, which can result in an umbilical hernia (an “outie” belly button). While this can be embarrassing and unsightly for many patients, tummy tuck surgery can restore the navel to an attractive, inward-facing appearance.
Umbilical hernias are most common with pregnant and postpartum women, and with people who are overweight. In adults, umbilical hernias typically don’t go away on their own and often grow larger over time.
I perform umbilical hernia surgery as part of tummy tuck surgery. I address umbilical hernias by making a tiny incision just above, below, or through the navel, depending on the exact location of the hernia, allowing me to push the hernia contents back into the abdomen and stitch together the fascia to close off the hernia. Various techniques can then be used to help restore a 3-dimensional shape to the belly button, which is often distorted by the hernia.
When performing umbilical hernia repair simultaneously with abdominoplasty, the blood supply to the belly button can sometimes be disrupted by the hernia or the hernia repair. Should the belly button become compromised—a relatively rare occurrence—a new one can be recreated.
Umbilical hernia surgery typically takes about 30 minutes irrespective of any other issues that need to be addressed during a tummy tuck.
8. Can I lose my belly button when undergoing diastasis recti repair surgery?
No—if you are working with a qualified plastic surgeon, your belly button will be carefully preserved during diastasis recti surgery. During a tummy tuck, your belly button stays in place, attached to the abdomen by the umbilical stalk, and is reinserted through the skin that has been shifted and tightened to create a smoother, flatter look. This can give the appearance that the belly button has moved slightly, but this is actually the result of fine surgical skill.
That said, there are some cases when I will leave the umbilicus intact at the skin level and detach the umbilical stalk to reposition the navel during diastasis recti surgery (this is known as an “umbilical float” tummy tuck). This is done much less commonly and under very specific circumstances, including cases where no significant excess skin needs to be removed.
(Please refer to Question 7 for an explanation of circumstances where the belly button may be compromised and need to be reconstructed).
9. What is your muscle repair technique for diastasis recti surgery?
Repairing diastasis recti during a tummy tuck allows me to tighten the abdominal wall and slim the waistline. Once I have sutured the abdominal muscles and connective fascia together, there’s typically some extra skin left over, which I trim to create a smooth, flat abdomen.
In nearly all cases, I am able to offer my patients a drainless tummy tuck, which allows them to avoid the use of cumbersome drains post-surgery. Instead of drains, a drainless tummy tuck maintains a patient’s Scarpa’s fascia (the deep connective tissue within your abdominal wall) during surgery, which acts as natural drainage for the lymphatic system.
A drainless tummy tuck allows my patients to recover faster and with fewer complications because their blood supply is improved and tissue damage is reduced.
Diastasis recti repair in BostonIf you believe you are suffering from diastasis recti, I invite you to schedule a consultation with me. I have been performing tummy tuck surgery in Boston for over 20 years and can help you achieve a flatter, firmer abdomen. Call (617) 786-7600 to discuss your diastasis recti options with me today.
